Smart Bandage Detects Bed Sores Before They are Visible
Author: University of California - Berkeley
Published: 2015/03/22 - Updated: 2017/11/06
Category Topic: Home Medical Devices - Related Publications
Contents: Synopsis - Introduction - Main
Synopsis: New smart bandage uses electrical currents to detect early tissue damage from pressure ulcers, or bedsores.
Introduction
Engineers at the University of California, Berkeley, are developing a new type of bandage that does far more than stanch the bleeding from a paper cut or scraped knee. Thanks to advances in flexible electronics, the researchers, in collaboration with colleagues at UC San Francisco, have created a new "smart bandage" that uses electrical currents to detect early tissue damage from pressure ulcers, or bedsores, before they can be seen by human eyes - and while recovery is still possible.
Main Content
"We set out to create a type of bandage that could detect bedsores as they are forming, before the damage reaches the surface of the skin," said Michel Maharbiz, a UC Berkeley associate professor of electrical engineering and computer sciences and head of the smart-bandage project.
"We can imagine this being carried by a nurse for spot-checking target areas on a patient, or it could be incorporated into a wound dressing to regularly monitor how it's healing."
The researchers exploited the electrical changes that occur when a healthy cell starts dying. They tested the thin, non-invasive bandage on the skin of rats and found that the device was able to detect varying degrees of tissue damage consistently across multiple animals.
Tackling a Growing Health Problem
The findings, published Tuesday, March 17, in the journal Nature Communications, could provide a major boost to efforts to stem a health problem that affects an estimated 2.5 million U.S. residents at an annual cost of $11 billion.
Pressure ulcers, or bedsores, are injuries that can result after prolonged pressure cuts off adequate blood supply to the skin. Areas that cover bony parts of the body, such as the heels, hips and tailbone, are common sites for bedsores. Patients who are bedridden or otherwise lack mobility are most at risk.
"By the time you see signs of a bedsore on the surface of the skin, it's usually too late," said Dr. Michael Harrison, a professor of surgery at UCSF and a co-investigator of the study. "This bandage could provide an easy early-warning system that would allow intervention before the injury is permanent. If you can detect bedsores early on, the solution is easy. Just take the pressure off."
Bedsores are associated with deadly septic infections, and recent research has shown that odds of a hospital patient dying are 2.8 times higher when they have pressure ulcers. The growing prevalence of diabetes and obesity has increased the risk factors for bedsores.
"The genius of this device is that it's looking at the electrical properties of the tissue to assess damage. We currently have no other way to do that in clinical practice," said Harrison. "It's tackling a big problem that many people have been trying to solve in the last 50 years. As a clinician and someone who has struggled with this clinical problem, this bandage is great."
Cells as Capacitors and Resistors
The researchers printed an array of dozens of electrodes onto a thin, flexible film. They discharged a very small current between the electrodes to create a spatial map of the underlying tissue based upon the flow of electricity at different frequencies, a technique called impedance spectroscopy.
The researchers pointed out that a cell's membrane is relatively impermeable when functioning properly, thus acting like an insulator to the cell's conductive contents and drawing the comparison to a capacitor. As a cell starts to die, the integrity of the cell wall starts to break down, allowing electrical signals to leak through, much like a resistor.
"Our device is a comprehensive demonstration that tissue health in a living organism can be locally mapped using impedance spectroscopy," said study lead author Sarah Swisher, a Ph.D. candidate in electrical engineering and computer sciences at UC Berkeley.
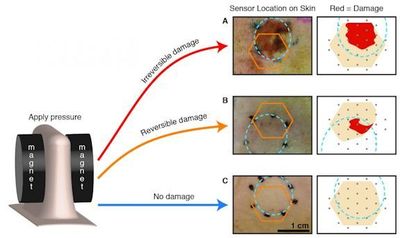
To mimic a pressure wound, the researchers gently squeezed the bare skin of rats between two magnets. They left the magnets in place for one or three hours while the rats resumed normal activity. The resumption of blood flow after the magnets were removed caused inflammation and oxidative damage that accelerated cell death. The smart bandage was used to collect data once a day for at least three days to track the progress of the wounds.
The smart bandage was able to detect changes in electrical resistance consistent with increased membrane permeability, a mark of a dying cell. Not surprisingly, one hour of pressure produced mild, reversible tissue damage while three hours of pressure produced more serious, permanent injury.
Promising Future
"One of the things that makes this work novel is that we took a comprehensive approach to understanding how the technique could be used to observe developing wounds in complex tissue," said Swisher. "In the past, people have used impedance spectroscopy for cell cultures or relatively simple measurements in tissue. What makes this unique is extending that to detect and extract useful information from wounds developing in the body. That's a big leap."
Maharbiz said the outlook for this and other smart bandage research is bright.
"As technology gets more and more miniaturized, and as we learn more and more about the responses the body has to disease and injury, we're able to build bandages that are very intelligent," he said. "You can imagine a future where the bandage you or a physician puts on could actually report a lot of interesting information that could be used to improve patient care."
Other lead researchers on the project include Vivek Subramanian and Ana Claudia Arias, both faculty members in UC Berkeley's Department of Electrical Engineering and Computer Sciences; and Shuvo Roy, a UCSF professor of bioengineering. Additional co-authors include Amy Liao and Monica Lin, both UC Berkeley Ph.D. students in bioengineering; and Yasser Khan, a UC Berkeley Ph.D. student in electrical engineering and computer sciences, who fabricated the sensor array. Study co-author Dr. David Young, UCSF professor of surgery, is now heading up a clinical trial of this bandage. The project is funded through the Flexible Resorbable Organic and Nano-material Therapeutic Systems (FRONTS) program of the National Science Foundation.