Definition of Back Pain Terms
Author: Lawrence Gold
Published: 2009/09/05 - Updated: 2022/02/09
Contents: Synopsis - Introduction - Main - Related Publications
Synopsis: Alphabetical list of definition covering the various terms used to describe the many different types of back pain.
Treatment for back pain generally depends on whether the pain is acute or chronic. In general, surgery is recommended only if there is evidence of worsening nerve damage and when diagnostic tests indicate structural changes for which corrective surgical procedures have been developed.
Introduction
About 80 percent of adults experience back pain at some point in their lifetimes. It is the most common cause of job-related disability and a leading contributor to missed work days. In a large survey, more than a quarter of adults reported experiencing low back pain during the past 3 months. The lower back where most back pain occurs includes the five vertebrae (referred to as L1-L5) in the lumbar region, which supports much of the weight of the upper body.
Main Content
Treatment for back pain generally depends on whether the pain is acute or chronic. In general, surgery is recommended only if there is evidence of worsening nerve damage and when diagnostic tests indicate structural changes for which corrective surgical procedures have been developed. This article discusses the following back pain terms (listed in alphabetical order):
- Back Injury vs. Spasm
- Bulging Disc
- Degenerative Disc Disease
- Disc Tear or Torn Disc
- Facet Joint Syndrome
- Herniated ("slipped") Disc
- Radiculopathy
- Ruptured Disc
- Sciatica, Referred Pain (Radiculopathy)
- Scoliosis
- Spinal Fusion
- Spinal Subluxations
Back Injury vs. Muscle Spasm
People commonly confuse spinal injuries with muscle spasms.
Spinal injuries involve changes in bone structure or soft-tissue consistency: fractured vertebrae, degenerating discs, torn or stretched ligaments, nerve damage. Spinal injuries require substantial healing time - or may never heal.
Muscle Spasms:
Painful muscular contractions - though painful, do not constitute an injury. Though symptoms of nerve impingement (tingling, burning, numbness, loss of muscular control) may accompany muscle spasms and mimic a spinal injury, these symptoms often disappear nearly instantly, once muscle spasms relax. Muscle spasms can often be induced to relax through somatic methods relatively quickly.
Muscle spasms often follow traumatic accidents, such as falls or motor vehicle mishaps, shocks to the nervous system that prompt the muscular system reflexively to tighten up. For that reason, muscle spasms may be confused with spinal (not "spinal cord") injuries. In persons with chronic muscular tension, muscle spasms may also occur when lifting heavy loads or even when bending forward, leading persons to speculate that they have injured their back.
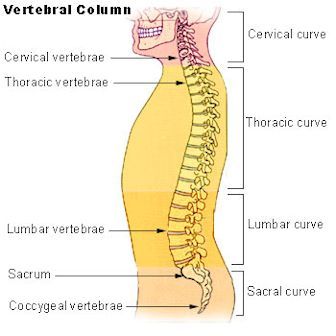
Fig. 2 Vertebral spinal column diagram.
Degenerative Disc Disease
Refers to breakdown of the inter-vertebral discs - the fibrocartilage spacers between vertebrae. The discs consist of two layers: a tough, fibrous outer ring or cylinder (annulus fibrosus) and a gelatinous core (nucleus pulposus).
Disc breakdown may range from mild disc bulge, to more severe disc bulge (herniation), to rupture of the disc with extrusion of disc material, to conversion of the disc into bone (fusion). This phenomenon may occur anywhere in the spine, including the neck.
While defined as a disease, Degenerative Disc Disease is no more a disease than a blowout of an overloaded tire is a disease of the tire. The breakdown comes from mechanical causes - over-compression.
Tight muscles of the back (the spinal extensors) pull neighboring vertebrae closer together, compressing the discs in between. Over time, the combination of over-compression and movement cause discs to break down, leading to the range of breakdown described above.
The breakdown process can be stopped by restoring normal pliancy to the spinal muscles and normal space between the vertebrae. Then, the healing process can restore disc integrity.
Added note:
Chronic dehydration due to insufficient water intake affects the discs adversely. As discs lose water, they lose plumpness and lose their ability to maintain space between neighboring vertebrae. Nerve entrapment, such as sciatica or tingling and numbness in the hands (including carpal tunnel syndrome), may result.
Disc Tear or Torn Disc
A consequence of violent injury, disc tear may appear symptomatically similar to a bulging disc but cannot be treated effectively by muscular retraining, traction, massage or other non-invasive techniques because the muscular contractions are protective in nature. The muscular contractions are stabilizing a length of spinal column that has lost its structural support.
A torn disc is a surgical situation. While surgery may restore stability to the spine, it may leave residual muscular contractions that must be addressed for recovery (and alleviation of symptoms) to be complete. Somatic education addresses such un-addressed muscular contractions.
Facet Joint Syndrome
The facet joints are bony projections on vertebrae. Generally, these bony projections on neighboring vertebrae don't touch each other, but muscular contractions along the spine pull neighboring vertebrae together and may cause those facet joints to meet with undue pressure and friction.
Another type of face joint exists where ribs meet vertebrae. Excessive tension of the muscles that control rib movement may also cause a kind of facet joint syndrome.
The pain and inflammation that result are sometimes called "facet joint syndrome" and sometimes, "spinal arthritis."
Herniated, Bulging, Slipped Disc
A sign of disc over-compression, the condition commonly arises when over-contracted back muscles shorten the spine along its length and pull vertebrae too close together for too long. The resulting disc compression causes the pulpy center (nucleus pulposus) of the disc (or discs) between neighboring vertebrae to push against the containing outer cylinder of the disc (annulus fibrosus). This compression causes bulging, much as overpressure on an overloaded tire causes bulging at the tire's weakest point.
Over time, the annulus fibrosus may break down under the compression force and the bulge increases or ruptures, pressing on the neighboring nerve root and causing pain and loss of function.
Relaxation of the over-contracted back muscles relieves the over-compression stress on spinal discs and in time allows discs to heal and regain their integrity.
Radiculopathy
This is another term familiar to physical therapists. It refers to tingling and numbness in the extremities that result from nerve impingement (a pinched nerve). The term implies damage to a nerve root where it exits the spinal column.
Sometimes, no damage exists; a nerve impingement of muscular origin exists. The symptoms of radiculopathy often disappear as soon as tensions of the spinal musculature normalize. Somatic procedures are generally rapidly effective. If after one-to-three sessions, substantial improvement has not occurred, you should seek further medical tests.
Referred Pain
This term, familiar to physical therapists, has to do with pinched nerves (nerve impingement). The term refers to pain at a location other than at the location where the nerve pinch exists. The sensation created by impingement (pinch) of the nerve "refers" to the region of the body where the nerve ending is, so the sensation is there, rather than at the site of the nerve pinch, itself - hence, "referred."
Sensory nerves end at brain connections corresponding to the body part they sense. A nerve that reports on the state of the foot ends in a brain connection that corresponds to the foot. That nerve "refers" to the foot.
If the nerve to the foot gets pinched, the brain interprets the nerve signal that results as a sensation of the foot. If the nerve that reports on the state of the buttock area gets pinched, the brain interprets the nerve signal as a sensation of the buttock.
Sciatica is an example of referred pain. The sciatic nerve branches down the back of the leg to the foot. A pinch or entrapment of the sciatic nerve at the waist or buttock (commonly caused by muscular tension) creates a signal that the brain interprets as trouble in the buttock, back of the leg or in the foot.
See Free of Back Pain or Outgrowing the Myth of Aging, two self-help programs that normalize muscular tensions that cause sciatica.
Ruptured Disc
A common end-point of disc herniation left untreated, a disc rupture extrudes the pulpy center of the disc (nucleus pulposus) out of the disc into the surrounding space outside the disc, like toothpaste out of a tube. The extruded disc material may then press upon nerve roots, causing referred pain.
A ruptured disc is generally a surgical situation. (Think "getting toothpaste back into the tube".) One minimally-invasive surgical procedure involves aspirating (sucking up) the extruded disc material.
While the procedure may relieve pressure on nerve roots, it leaves the muscular contractions underlying the problem un-addressed. Somatic education deals with such un-addressed muscular contractions.
Scoliosis
Abnormal curvature of the spine. While a normal spine exhibits curves and the natural curvability that allow flexibility, some people exhibit spinal curvatures that interfere with normal movement and distort posture.
Scoliosis has been classified into several categories that describe type of curvature and degree of severity. Without going into detail about the varieties of scoliosis, it can be said in general that scoliosis can be classified into "structural" and "functional" types. Structural scoliosis involves distortions of bone growth. While not correctable by non-surgical means, some procedures can improve comfort and mobility within the limits of the scoliosis. Functional scoliosis arises from muscular pulls that may arise from injury and subsequent casting of an extremity. It is often correctable by non-surgical means (see below).
Common medical treatments for scoliosis involves casting, the wearing of a brace, insertion of metal rods along the spine, or spinal fusion surgery.
In some cases, less drastic, non-medical means are equally effective without inflicting the trauma or lifelong limitations that medical procedures impose. Somatic training can sometimes correct even complex scoliosis by correcting the imbalances of muscular pulls. At other times, more may be needed, particularly if the supportive connective tissue is displaced from its normal position and span. Then, a combination of myofascial integration (soft-tissue manipulation) techniques (such as Rolfing or Hellerwork) plus somatic training (such as Hanna Somatic Education) is needed. Interestingly, with the combination of soft-tissue manipulation techniques and muscular retraining, the body's own soft-tissue and muscular system provide the support otherwise provided by casting or bracing.
Spinal Fusion
A surgical procedure, spinal fusion is a man-made way of recreating a natural end-process of disc breakdown: the growth of bone to replace degenerated discs. In the procedure, the ridges (spinous processes) and rear wall (laminae) of vertebrae are surgically removed (laminectomy), the disc or discs removed, bony material (generally the size and shape of matchsticks) placed to grow over the surgical wound, and the patient placed in a torso cast. The result is a rigid spine incapable of its normal flexibility, but stabilized to prevent nerve impingement. Pain sometimes remains due to reflexive muscular contractions at the surgical site.
Spinal fusion is considered a last-measure procedure employed in "emergency" cases, as determined by symptomology and radiological examination, generally with patients for whom physical therapy has failed or who have had traumatic injury. In some cases, it is unavoidable; in other cases (scoliosis), less aggressive surgical means combined with somatic education can produce a satisfactory outcome.
Spinal Subluxations
The term, "subluxation," originally coined by D.D. Palmer, refers to a blockage of light ("lux") through the length of the spinal cord by misalignments of neighboring vertebrae. Such misalignments adversely affect posture, movement, and organ function by affecting nerve signal transmission. The original meaning of the term is no longer used in public discourse about chiropractic.
Bones go where muscles pull them. Abnormal (habituated) tensions in the spinal muscles pull vertebrae out of alignment. As muscular functioning normalizes, spinal alignment usually normalizes spontaneously.
Without normalization of muscular functioning, spinal misalignments tend to return; with normalization of muscular functioning, chiropractic adjustments, if needed, tend to be long-lasting and are needed less often, if ever.
Reference
Lawrence Gold is a long-time practitioner of Hanna somatic education published in the American Journal of Pain Management (January, 1996, Vol. 6, no. 1, pg. 30) and the Therapeutic Specialist's Quarterly Report (summer, 1997, Vol. II, Issue VI, pg. 2).