Arachnoiditis: Diagnosis, Pain Sources, Cause, Treatments
Author: Thomas C. Weiss
Published: 2014/11/12 - Updated: 2021/10/17
Contents: Synopsis - Introduction - Main - Related Publications
Synopsis: Information regarding arachnoiditis, a pain disorder caused by inflammation of the arachnoid, a membrane that surrounds and protects nerves in the spinal cord.
The disorder is characterized by severe stinging, burning pain and neurological issues. Arachnoiditis has no consistent pattern of symptoms, yet in many people it affects the nerves connecting to the lower back and legs.
Introduction
What is Arachnoiditis?
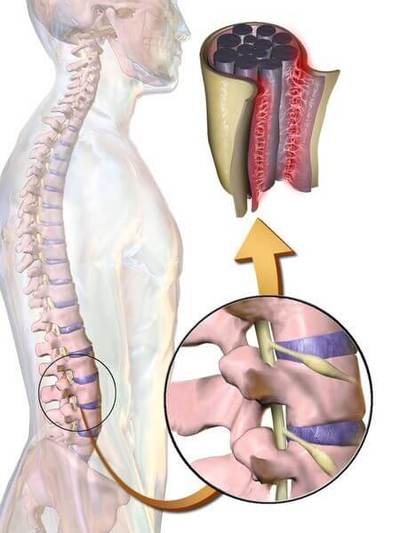
Arachnoiditis is an inflammation of the arachnoid, one of the membranes known as meninges that surround and protect the nerves of the central nervous system, including the brain and spinal cord. The arachnoid can become inflamed because of adverse reactions to chemicals, infection from bacteria or viruses, as the result of direct injury to the spine, chronic compression of spinal nerves, complications from spinal surgery or other invasive spinal procedures, or the accidental intrathecal injection of steroids intended for the epidural space. Arachnoiditis is difficult to treat. Treatment is limited to alleviation of pain and other symptoms. Surgical intervention generally has a poor outcome, and only provides temporary relief. Steroid injections, administered either intrathecally or epidurally have been linked as a cause of the disease, therefore they are generally discouraged as a treatment and may even worsen the condition. Doctors have different views about this disease so seeking a second opinion may be wise.
Main Content
The disorder is characterized by severe stinging, burning pain and neurological issues. Arachnoiditis has no consistent pattern of symptoms, yet in many people it affects the nerves connecting to the lower back and legs. The most common symptom is pain, although the disorder may also cause the following:
- Bladder, bowel and/or sexual issues
- Tingling, numbness, or weakness in the legs
- Muscle cramps, spasms and uncontrollable twitching
- Severe shooting pain that can be similar to an electric shock sensation
- Sensations that might feel like insects crawling on the skin, or water trickling down the leg
As the disease progresses, symptoms may become more severe or permanent. A number of people with arachnoiditis are unable to work and experience significant disability because they are in constant pain.
Arachnoiditis Causes
Inflammation of the arachnoid may lead to the formation of scar tissue and can cause the spinal nerves to stick together and malfunction. The arachnoid may become inflamed because of an irritation from one of the sources below:
- Direct injury to the spine
- Complications from spinal surgery or other invasive spinal procedures
- Infection from bacteria or viruses such as viral or fungal meningitis which may affect the spine
- Chronic compression of spinal nerves - causes for this compression include advanced spinal stenosis or chronic degenerative disease
Dye used in myelograms have also been blamed for some instances of arachnoiditis. The radiographic contrast media responsible for this is not used anymore. There is also concern that the preservatives found in epidural steroid injections may cause arachnoiditis.
Arachnoiditis Diagnosis
Diagnosing arachnoiditis can be hard, yet tests such as a CAT scan or MRI have helped with diagnosing the disorder. A test called an, 'electromyogram (EMG),' can assess the severity of the ongoing damage to affected nerve roots by using electrical impulses to check nerve function.
Causes of Pain in Arachnoiditis Syndrome
People who experience arachnoiditis syndrome might present with different combinations of back, leg and buttock pain as well as muscle weakness, numbness and widespread, 'Dysaesthaesia.' It takes the form of diffuse and often times intense pain across the person's back, spreading up to the thoracic spine, down to involve the person's sacrum and coccyx, deeply into the person's pelvis or perineum and extensively down one or both of the person's legs. The symptoms may present as pins and needles, a sense of ants crawling up and down the body, or cold or scalding water sensations.
A number of doctors will reach for a psychological or arachnoiditic explanation for the person's symptoms. In fact - the MRI scan might show the presence of a dehydrated disc, possibly with a High Intensity Zone or leaking disc wall tear. The source can be confirmed spinal probing and discography in the aware state with the symptoms being compounded by the presence of scarring induced by a reaction to these leaking products. Misdiagnosis prevents people from receiving definitive endoscopic minimally invasive spine surgery and they usually find themselves referred for palliative chronic pain management.
Neck pain with arm symptoms may also occur on rare occasions. The pains appear to emanate from inflammation at the lower lumbar spine, presumably transmitted through the posterior longitudinal ligament and secondary cervical malposture. The assumption is made because the symptoms settle by treatment of the person's L4/5 and L5/S1 disc levels by endoscopic minimally invasive spine surgery and muscle balance physiotherapy.
Pinpointing Pain Sources
Aware state surgical examination enables a person to provide the surgeon with feedback, guiding the surgeon to the point that is responsible for the pain. The, 'live,' approach allows the causal level in people with arachnoiditis syndrome to be accurately defined and then the source of the pain outside the dura to be viewed and addressed using endoscopic instruments through a tiny incision. In this way, neural anomalies and strange nerve combinations may be detected and diagnostic errors regarding the disc level responsible for the person's pain to be avoided. The surgeon is guided to the precise source of the person's pain at the specified inter-vertebral point and an understanding of the actual mechanisms underlying the cause.
Arachnoiditis Treatment
There is currently no cure for arachnoiditis. Treatment options for arachnoiditis are similar to those for other chronic pain conditions. Most treatments concentrate on relieving pain and improving symptoms that impair a person's daily activities. Often, health care professionals recommend a program of pain management, exercise, physiotherapy, as well as psychotherapy. Surgery for arachnoiditis is controversial because outcomes may be poor and provide only short-term relief for the person. Clinical trials of steroid injections and electrical stimulation are needed to determine whether those treatments are effective.
Accurately Targeted Treatment
Single targeted surgery enabled people with arachnoiditis to be precisely treated with a minimum of damage to their tissues, reduced patient risk, enhanced long-term outcome and more without the use of a general anesthesia. The treatment is called, 'foraminoplasty,' because it is carried out in the gaps or, 'foramen,' between a person's vertebrae and allows the person's nerve to be liberated and the overriding joints or pointed fracture margins to be removed. The treatment is only possible by the use of endoscopic minimally invasive spine surgery where the full length of the exiting nerve may be explored and the points of irritation clearly demonstrated. In the breadth of presentations arising from degenerative disc disease and failed back surgery, or failed chronic pain management causing the inflammation outside the dura, endoscopic lumbar decompression and foraminoplasty achieved a successful positive outcome in around 80% of those affected.
Conventional Surgery Issues
The use of multi-level open surgery in arachnoiditis including decompression, microdiscectomy, solid or flexible fusion is considered to be, 'overkill,' and risks increasing the degree of clumping with negative side-effects including potential nerve and tissue damage, blood loss, extended post-operative care and unnecessarily operating on pain-free levels. It is fraught with aggravation of the person's current symptom status. Conventional surgery is not as effective as foraminoplasty in addressing and ameliorating the effects of arachnoiditis. Instead, it runs the risk of increased neurological combinations as well as causing complications of recurrent disc bulging, nerve damage, infection, scarring around the nerve, major vessel damage, implant failure or sexual dysfunction.
 Author Credentials: Thomas C. Weiss is a researcher and editor for Disabled World. Thomas attended college and university courses earning a Masters, Bachelors and two Associate degrees, as well as pursing Disability Studies. As a CNA Thomas has providing care for people with all forms of disabilities. Explore Thomas' complete biography for comprehensive insights into his background, expertise, and accomplishments.
Author Credentials: Thomas C. Weiss is a researcher and editor for Disabled World. Thomas attended college and university courses earning a Masters, Bachelors and two Associate degrees, as well as pursing Disability Studies. As a CNA Thomas has providing care for people with all forms of disabilities. Explore Thomas' complete biography for comprehensive insights into his background, expertise, and accomplishments.