Antidepressant Use: Increased Risk of Type II Diabetes
Author: Thomas C. Weiss
Published: 2013/10/01 - Updated: 2021/08/31
Contents: Synopsis - Introduction - Main - Related Publications
Synopsis: Increased risk of type 2 diabetes associated with weight gain among people who used antidepressants over the long-term than in people matched for depression-related characteristics.
An analysis of people who used antidepressants less than or equal to 200 daily doses within one year and people who did not use antidepressants replicated the excess risk associated with the long-term use of antidepressants.
Introduction
A recent study suggests the use of antidepressants might increase a person's risk of developing type 2 diabetes. Frank B. Hu of Harvard School of Public Health and his colleagues conducted the analysis and discovered that using antidepressant medications was associated with a 68% increased risk for developing type 2 diabetes. Prior studies have associated the use of antidepressants with type 2 diabetes.
Main Content
Antidepressants are drugs used for the treatment of clinical depression and other conditions, including anxiety disorders, obsessive compulsive disorder, eating disorders, chronic pain, neuropathic pain and, in some cases, dysmenorrhea, snoring, migraines, attention-deficit hyperactivity disorder (ADHD), substance abuse and sleep disorders. They can be used alone or in combination with other medications.
The latest study was based on 3 cohorts of American adults participating in the, 'Health Professionals Follow-Up Study,' women in the, 'Nurses' Health Study I,' and women in the, 'Nurses' Health Study II.' At baseline, every participant was free of type 2 diabetes, cancer, or cardiovascular disease. The baseline ages for participants 56.4, 61.3 and 38.1 years respectively. People were surveyed at baseline and every 2 years for their use of antidepressants.
Through 1,644,679 person-years of follow-up researchers found 6,641 cases of type 2 diabetes. People who used antidepressants were at 68% increased risk of type 2 diabetes. The risk increased by 30% among people who used antidepressant medications after adjustment for other risk factors for diabetes and history of hypertension and high cholesterol. After adjustment for body mass index, the risk increased 17%.
Use of selective serotonin reuptake inhibitors and other antidepressants were correlated with 10% and 26% increased risk for type 2 diabetes. Researchers concluded that people who use antidepressants had a moderately elevated risk of type 2 diabetes when compared with those who do not, even after adjustment for body mass index. Side effects of antidepressant medications may include:
- Anxiety
- Nausea
- Agitation
- Dizziness
- Headache
- Dry mouth
- Drowsiness
- Weight gain
- Constipation
Type 2 diabetes affects millions of people in America. There is currently no cure for it, yet the disease may be managed by taking prescription medications and long-term dietary intervention. Some non-conventional remedies such as cinnamon and curcumin may help treat or prevent diabetes.
'Absolute Risk,' and Diabetes
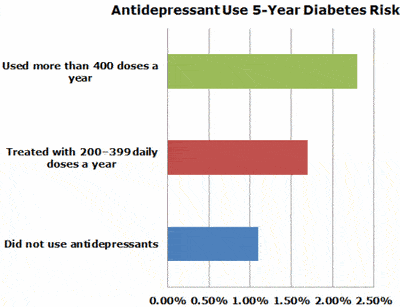
An analysis of people who used antidepressants less than or equal to 200 daily doses within one year and people who did not use antidepressants replicated the excess risk associated with the long-term use of antidepressants. For 5 years, the absolute risk of incident diabetes was 1.8% for people who used the medications and 1.1% for people who did not. The corresponding absolute risk estimate for people treated with 200-399 daily doses a year was 1.7%, while for people who took in excess of 400 doses of antidepressant medications experienced an absolute risk of developing diabetes of 2.3%.
The relative risk estimates for incident diabetes associated with antidepressant use of 200-399 daily doses per year and more than 400 compared with no use of the medications were 1.53 and 2.00 respectively. There was a separation of survival curves between antidepressant users of more than 200 doses per year and those who did not across the entire follow-up period. The findings are significant.
Analysis of data drawn from a cohort of more than 150,000 adults showed a series of important results. Antidepressant medication use was associated with a doubling of the risk of being diagnosed with type 2 diabetes, despite a record of severe depression. The excess risk associated with antidepressant use was observable for both SSRI's and tricyclic antidepressants. In absolute terms, the 5 year risk of being diagnosed with diabetes increased in a, 'dose-response fashion,' depending upon a person's level of exposure to the medication:
- 1.1% in people who did not use antidepressants
- 1.7% among people treated with 200-399 daily doses a year
- 2.3% among people using more than or equal to 400 doses a year
Supporting biological plausibility of this association, weight gain was more rapid among people who used antidepressants over the long-term than in people matched for depression-related characteristics.
The findings add to existing evidence from other studies. In the randomized Diabetes Prevention Program of pre-diabetic individuals, the use of antidepressants at baseline was associated with an increased risk of type 2 diabetes at follow-up, whereas self-reported depressive symptoms at baseline were not predictive of diabetes risk. An analysis of the medical records of people with depression from the U.K. General Practice Research Database discovered that long-term use of antidepressants with high or moderate daily doses was associated with an increased risk of diabetes, yet treatment with lower daily doses was not. The study took into account dose and duration of antidepressant use as well as baseline status of severe depression.
Additional studies have reported inconsistent findings.
A Norwegian cross-sectional health survey, a study of spontaneous reports listed in the World Health Organization Adverse Drug Reaction Database, and an analysis of data from a province in Canada all found support for an association between the use of antidepressant medications and diabetes. In a sample of adults age 55, treatment with antidepressants was not associated with an increased risk of diabetes, yet the study lacked adequate statistical power because the number of antidepressant users who developed diabetes was only 4. Analysis using prescription data from the PHARMO database in the Netherlands did not find an increased risk of diabetes among people using antidepressants. It is important to note that this particular study did not take into consideration the duration or dose of antidepressants in treatment. Other studies suggest that inclusion of short-term or low-dose treatment with antidepressants is likely to dilute the association.
Weight gain was greater among people who used antidepressants than among those who did not.
A prior trajectory analysis of repeat body-mass index measurements found an average of 0.03 unit faster increase in body-mass index among people who later developed type 2 diabetes when compared with people who remained free of diabetes. What this translates to is 0.1kg of excess weight gain per year for people with incident diabetes. It suggests that antidepressant medication use is related to 0.3kg of excess weight gain per year, which is a change large enough to contribute to a person's diabetes risk. The findings agree with prior studies confirming that antidepressants may induce weight gain and promote hyperglycemia, showing that SSRI use is associated with an increased risk of weight gain in the long-term.
 Author Credentials: Thomas C. Weiss is a researcher and editor for Disabled World. Thomas attended college and university courses earning a Masters, Bachelors and two Associate degrees, as well as pursing Disability Studies. As a CNA Thomas has providing care for people with all forms of disabilities. Explore Thomas' complete biography for comprehensive insights into his background, expertise, and accomplishments.
Author Credentials: Thomas C. Weiss is a researcher and editor for Disabled World. Thomas attended college and university courses earning a Masters, Bachelors and two Associate degrees, as well as pursing Disability Studies. As a CNA Thomas has providing care for people with all forms of disabilities. Explore Thomas' complete biography for comprehensive insights into his background, expertise, and accomplishments.