Embryonic Selection by Polygenic Scores and Disability
Author: Ian C. Langtree - Writer/Editor for Disabled World (DW)
Published: 2026/02/23
Publication Type: Informative
Category Topic: Journals - Papers - Related Publications
Contents: Synopsis - Introduction - Main - Insights, Updates
Synopsis: The promise of choosing healthier embryos through genetic scoring has captivated prospective parents and alarmed ethicists in equal measure. Embryonic selection based on polygenic scores represents one of the most consequential - and contentious - advances in reproductive technology, raising fundamental questions about the limits of parental choice, the reliability of genetic prediction, and what it means to value human diversity in an era when the building blocks of life can be read like a probabilistic spreadsheet.
- Topic Definition: Embryonic Selection
Embryonic selection is the process by which one or more embryos created through in vitro fertilization are evaluated and chosen for transfer to the uterus based on specific genetic or chromosomal criteria. This can involve screening for chromosomal abnormalities, single-gene disorders linked to known family histories, or - more recently and controversially - polygenic risk scores that estimate an embryo's statistical likelihood of developing common complex conditions or displaying particular traits later in life. The goal is to give prospective parents information that may help them select an embryo with a more favorable health outlook, though the process raises significant scientific, ethical, and social questions about the reliability of genetic prediction and the broader implications of choosing among potential future people on the basis of their DNA.
Introduction
Embryonic Selection Based on Polygenic Scores: Science, Ethics, and the Disability Debate
The ability to peer into an embryo's genetic code and predict its future health has long been a fixture of science fiction. But in recent years, that fiction has started to become reality. Companies in the United States and elsewhere have begun offering a service known as embryonic selection based on polygenic scores, or ESPS, to prospective parents undergoing in vitro fertilization (IVF). The technology promises to help parents choose embryos with lower genetic risk for common diseases - and, in some cases, with traits like higher predicted intelligence or taller stature. Yet as the science races ahead, serious questions about accuracy, fairness, and the very meaning of disability are demanding answers.
Main Content
What Are Polygenic Scores?
To understand embryonic selection based on polygenic scores, you first need to understand polygenic scores themselves. Unlike conditions caused by a single gene mutation - such as cystic fibrosis or sickle cell disease - most common diseases and human traits are influenced by thousands of genetic variants scattered across the genome. Heart disease, type 2 diabetes, schizophrenia, height, and even educational attainment are all shaped by this kind of complex, distributed genetic architecture.
A polygenic score (also called a polygenic risk score, or PRS) is essentially a statistical summary. Researchers study massive databases of adult genomes through what are called genome-wide association studies (GWAS), identifying which genetic variants are slightly more common among people who develop a particular condition or display a particular trait. By tallying up the effects of hundreds or thousands of these tiny genetic nudges in a single individual, scientists can produce a score that estimates that person's genetic predisposition toward a given outcome (Turley et al., 2021).
It is important to note that these scores are probabilistic, not deterministic. A high polygenic score for diabetes does not mean a person will develop diabetes. It means they may have a somewhat elevated genetic risk compared to someone with a lower score. Environment, lifestyle, and countless other factors play enormous roles in whether any particular condition actually develops.
How ESPS Works in Practice
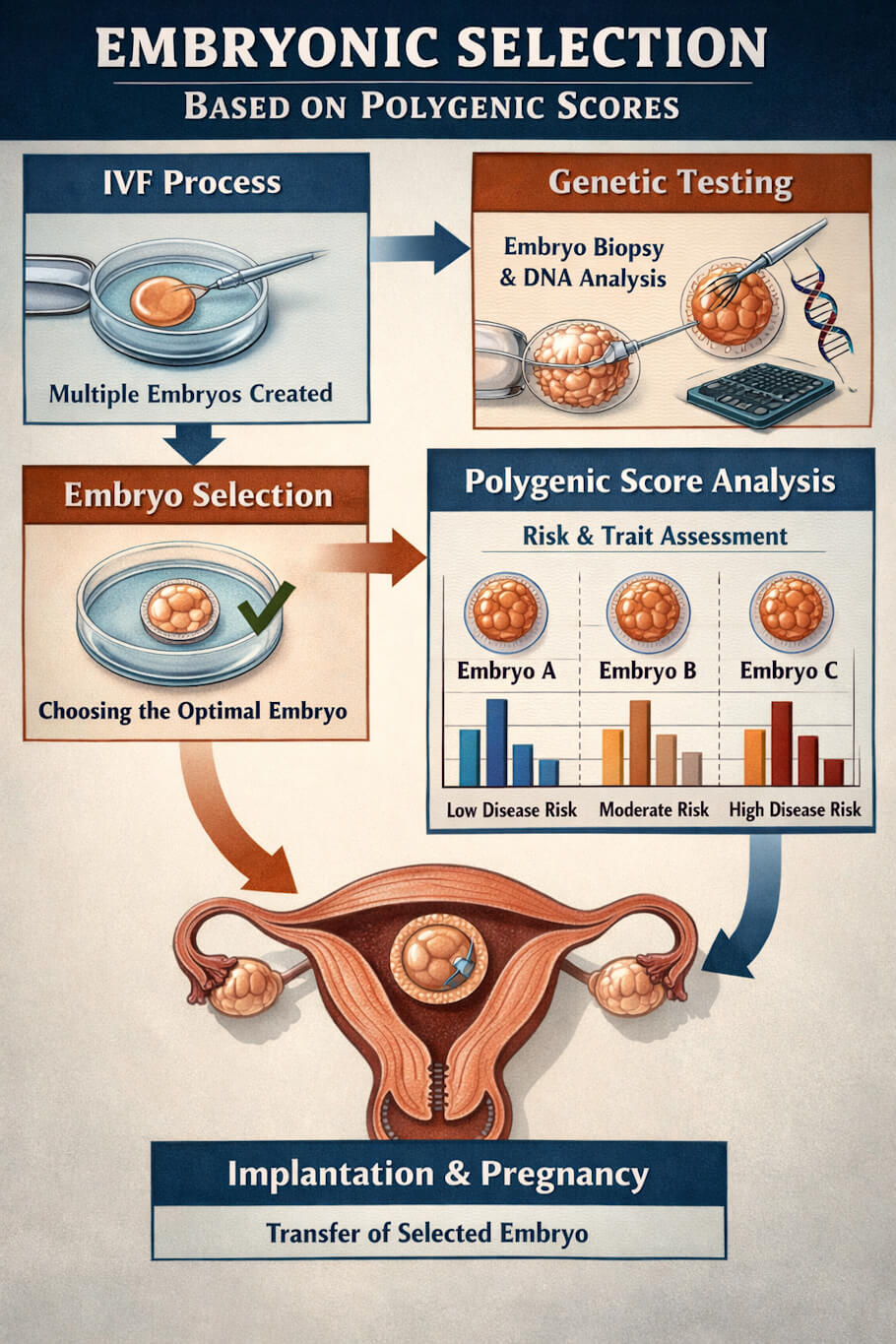
In a typical IVF cycle, multiple embryos are created through the fertilization of eggs in a laboratory. Traditionally, embryos have been screened for chromosomal abnormalities (such as extra or missing chromosomes) and for single-gene disorders when there is a family history of a specific condition. Embryonic selection based on polygenic scores adds a new layer to this process.
During ESPS, a small number of cells are biopsied from each embryo at the blastocyst stage - usually around five days after fertilization. These cells are then genotyped, meaning their DNA is analyzed to identify hundreds of thousands of genetic variants. Using algorithms derived from GWAS data, polygenic scores are calculated for each embryo across one or more conditions. Parents can then theoretically select the embryo with the most favorable genetic risk profile for implantation (Karavani et al., 2019).
Several companies have entered this space. Genomic Prediction, a New Jersey-based firm, was among the first to commercially offer what it calls "LifeView" testing. The first baby reportedly born after polygenic embryo screening arrived in 2020, with the embryo selected for having the lowest predicted genetic risk for conditions including heart disease, diabetes, cancer, and schizophrenia. Since then, other startups have followed, and the number of children born following this kind of screening is believed to be in the hundreds, though exact figures remain unclear (Polyakov et al., 2022).
The Scientific Limitations
While the concept sounds powerful, the scientific community has raised significant concerns about how well polygenic scores actually perform in the context of embryo selection. A landmark 2021 report in the New England Journal of Medicine laid out several reasons why the technology may not deliver on its promises (Turley et al., 2021).
The first major issue is that polygenic scores developed from studies comparing people across different families lose much of their predictive power when applied to siblings - which is exactly the comparison that matters in embryo selection. When you are choosing among embryos from the same two parents, the genetic differences between those embryos are much smaller than the differences between unrelated individuals in a population study. The expected gain from choosing the embryo with the highest polygenic score for educational attainment, for instance, was estimated at roughly half a year of additional schooling when the correct within-family calculation was applied - far less dramatic than the figures sometimes suggested in marketing materials (Turley et al., 2021).
A second concern involves ancestral bias. The vast majority of GWAS have been conducted on populations of European descent. When polygenic scores derived from these studies are applied to embryos from parents of other ancestral backgrounds, their accuracy drops substantially. This means the technology is likely to be least reliable for the communities that already face the greatest health disparities (Martin et al., 2019).
Third, there is the problem of pleiotropy - the fact that individual genetic variants often influence multiple traits simultaneously. Selecting an embryo for lower risk of one condition might inadvertently increase risk for another. The New England Journal of Medicine report noted, for example, that genetic variants associated with higher educational attainment also tend to be associated with increased risk for bipolar disorder. This creates genuinely difficult trade-offs that prospective parents may not fully appreciate (Turley et al., 2021).
Finally, the number of viable embryos available in any given IVF cycle is typically small - often fewer than five - which sharply limits the range of genetic variation parents can actually choose from. The likelihood that any one couple will produce embryos with dramatically different polygenic scores is quite low (Karavani et al., 2019).
Professional and Institutional Positions
The medical establishment has largely urged caution. In December 2025, the American Society for Reproductive Medicine (ASRM) published a joint report from its Ethics and Practice Committees concluding that preimplantation genetic testing for polygenic disorders (PGT-P) is not ready for clinical practice and should not be offered as a reproductive service. The report cited insufficient predictive accuracy, incomplete understanding of gene-environment interactions, and a lack of diverse population data as key reasons (ASRM, 2025).
Similarly, the American College of Medical Genetics and Genomics (ACMG) released a points-to-consider statement in 2024 cautioning that the technology was advancing faster than the evidence supporting its clinical utility. The International Society of Psychiatric Genetics (ISPG) issued its own statement expressing particular concern about the use of polygenic scores to screen embryos for psychiatric conditions, noting that such scores do not determine whether a person will develop a condition and that screening for psychiatric traits may increase stigma (Lencz et al., 2022).
ESPS and Disability: The Heart of the Ethical Debate
Perhaps no dimension of this technology sparks more passionate debate than its relationship to disability. For many disability rights advocates, polygenic embryo screening represents a troubling extension of long-standing practices that treat disability as something to be eliminated rather than accommodated.
The concern is sometimes framed as what ethicists call the "expressivist objection." The argument goes something like this: when prospective parents screen embryos to reduce the likelihood of conditions associated with disability - whether physical, cognitive, or psychiatric - the implicit message is that lives lived with those conditions are less valuable or less worth living. Even when individual parents are acting out of love and concern for their future child, the cumulative effect of widespread screening could be to reinforce harmful stereotypes and reduce the diversity of human experience (Lazaro-Munoz et al., 2021).
This concern is not hypothetical. Research has consistently shown that people without disabilities tend to underestimate the quality of life experienced by people who do have disabilities. Many individuals living with conditions like Down syndrome, autism, or bipolar disorder report rich and fulfilling lives - a reality that rarely figures into clinical conversations about genetic screening. Multiple studies have also found that physicians tend to hold more negative views of life with disability than disabled individuals themselves, creating a systemic tilt toward screening and selection (Miller and Levine, 2013).
The Autism Example
The autism community provides a particularly instructive case study. Many autistic self-advocates have expressed deep concern that polygenic screening could be used to select against embryos with a higher genetic likelihood of developing autism. From a neurodiversity perspective, autism is understood not as a disease to be prevented but as a natural form of neurological variation that comes with both challenges and strengths. The fear is that polygenic screening - even if framed as a health measure - could undermine decades of progress in establishing that autistic lives have equal value and dignity (Lencz et al., 2022).
Some stakeholders have drawn parallels to the experience of the Deaf community, which has long resisted the framing of deafness as a deficit requiring medical correction. The concern is that as polygenic scores become more refined, the range of human variation targeted for selection could steadily expand, moving from severe medical conditions to traits that many within affected communities view as fundamental aspects of their identity.
Psychiatric Conditions and Stigma
Polygenic embryo screening also raises particular concerns in the context of psychiatric conditions. Schizophrenia, bipolar disorder, and major depression are already among the conditions for which commercial screening is available. Disability advocates and psychiatric geneticists alike have warned that screening embryos for psychiatric risk may deepen the stigma already faced by people living with mental health conditions. The ISPG's 2021 statement specifically flagged this concern, noting that psychiatric genetics has a troubling historical entanglement with eugenic ideology (Lencz et al., 2022).
The heterogeneity of psychiatric conditions makes this especially fraught. Two people with schizophrenia may have vastly different life experiences and functional outcomes. A polygenic score cannot capture this variability. It can only assign a statistical probability that tells parents very little about what their child's actual lived experience would be.
The Pros of Embryonic Selection Based on Polygenic Scores
Despite these concerns, proponents of the technology point to several potential benefits that deserve honest consideration.
Reducing Disease Burden
The most straightforward argument in favor of ESPS is the possibility of reducing the lifetime burden of serious disease. Conditions like type 2 diabetes, coronary artery disease, and certain cancers cause enormous suffering and carry significant costs for individuals and healthcare systems. If polygenic screening can even modestly shift the odds in favor of better health outcomes, some argue, parents should have the option to use it (Savulescu, 2007).
Reproductive Autonomy
Many advocates frame ESPS as an extension of reproductive autonomy - the principle that individuals should have the freedom to make informed decisions about their own reproduction. Parents already make choices about prenatal care, nutrition, and environment that influence their children's outcomes. From this perspective, using available genetic information to guide embryo selection is a natural extension of responsible parenting, not a eugenic overreach.
Prevention Without Alteration
Unlike gene editing technologies such as CRISPR, polygenic embryo screening does not modify the genome. It simply involves choosing among naturally conceived embryos based on existing genetic variation. For some, this distinction matters ethically - the technology does not create anything artificial but rather helps parents make more informed choices among the embryos they have already produced.
The Cons of Embryonic Selection Based on Polygenic Scores
The objections to ESPS are numerous and cut across scientific, ethical, and social domains.
Unreliable Predictions
As discussed earlier, the predictive accuracy of polygenic scores in the embryo selection context is significantly lower than marketing materials may suggest. The gap between relative risk reduction and absolute risk reduction is substantial. While companies may report relative risk reductions of 15 to 80 percent for certain conditions, the absolute risk reductions have been estimated at only 0.12 to 8.5 percent for people of European ancestry - and even less for other ancestral backgrounds (Turley et al., 2021).
Exacerbating Inequality
IVF is already expensive, and adding polygenic screening increases the cost further. If ESPS delivers even modest health advantages, those advantages will be disproportionately available to wealthier families. Over time, this could widen existing health disparities along socioeconomic lines. The ancestral bias in current polygenic scores compounds this problem, meaning the technology works less well for precisely the populations that already face the greatest health inequities (Martin et al., 2019).
The Shadow of Eugenics
The historical specter of eugenics looms large over this technology. The early twentieth century eugenics movement, which led to forced sterilization programs and ultimately contributed to the ideological framework behind the Holocaust, was also promoted with progressive, well-intentioned language about improving human welfare. While modern polygenic screening is voluntary and individual rather than coercive and state-sponsored, critics argue that the underlying logic - that certain genetic profiles are more desirable than others - carries echoes of that darker history (Lombardo, 2018).
At least one founder of a company offering polygenic embryo screening has publicly speculated about eventually offering screening for traits like skin color and above-average cognitive ability in certain countries. Such possibilities underscore why many ethicists believe that the technology requires robust regulatory oversight before its use expands further (Turley et al., 2021).
Undermining the Value of Disabled Lives
As explored earlier, widespread screening against traits associated with disability sends a message about whose lives are considered worth living. This is not merely a philosophical concern. Practical consequences can follow, including reduced funding for disability services and support, diminished community solidarity, and increased pressure on parents who choose not to screen. The disability rights community has been particularly vocal about the danger of allowing market-driven genetic selection to gradually narrow the range of human variation that society considers acceptable.
Informed Consent Challenges
The complexity of polygenic risk information creates real problems for informed consent. Healthcare professionals in reproductive medicine have expressed concern that patients may not fully understand what polygenic scores can and cannot tell them. The risk of false expectations is significant - parents may believe they are selecting a "healthy" embryo when in reality they are choosing among options with only marginally different risk profiles. In one documented case, a couple who learned that two of their five embryos had elevated polygenic risk for breast cancer decided against implanting any of them - a decision that illustrates how complex and emotionally fraught these choices can become (Lazaro-Munoz et al., 2021).
Regulation and the Path Forward
One of the most striking aspects of polygenic embryo screening is how little regulatory oversight currently governs its use. In the United States, there is no specific regulation of ESPS. Most European countries restrict genetic testing of embryos to serious medical conditions, but enforcement varies and the technology exists in a gray area in many jurisdictions. South Africa, for instance, regulates embryonic screening under its National Health Act, but the regulations do not specifically address polygenic scoring (Hastings Center, 2021).
The 2021 New England Journal of Medicine report called on the Federal Trade Commission to develop standards for how companies communicate about ESPS, particularly with respect to the distinction between relative and absolute risk reduction. The authors also called for a broader societal conversation about whether the technology should be limited to medical applications or permitted for non-disease traits as well (Turley et al., 2021).
As polygenic scores become more accurate and the cost of genetic sequencing continues to fall, the pressure to use this technology will likely increase. The decisions that societies make now about oversight, access, and ethical boundaries will shape the reproductive landscape for generations to come. Finding a path that respects individual reproductive freedom while protecting the values of diversity, equity, and human dignity is one of the defining challenges of modern bioethics.
Conclusion
Embryonic selection based on polygenic scores sits at a complicated intersection of cutting-edge genetics, reproductive medicine, personal choice, and social values. The technology holds real, if currently modest, potential to reduce the burden of common diseases. But it also raises profound questions about who gets to decide what counts as a desirable human life, and about the kind of society we are building when we treat genetic risk profiles as the basis for selecting future people.
For the disability community, the stakes could not be higher. The history of eugenics offers a sobering reminder that well-intentioned efforts to improve human health can slide into something far less benign when coupled with assumptions about which lives are worth living. As this technology continues to evolve, the voices of disabled individuals, psychiatric survivors, neurodiversity advocates, and other affected communities must be central to the conversation - not an afterthought. The question is not simply whether we can screen embryos for polygenic traits. The question is whether, and under what conditions, we should.
References
- American Society for Reproductive Medicine. (2025). ASRM Ethics and Practice Committees release new report concluding polygenic embryo screening is not ready for clinical use. Fertility and Sterility.
- Karavani, E., Zuk, O., Zeevi, D., Barzilai, N., Stefanis, N. C., Hatzimanolis, A., ... and Carmi, S. (2019). Screening human embryos for polygenic traits has limited utility. Cell, 179(6), 1424-1435.
- Lazaro-Munoz, G., Pereira, S., Carmi, S., and Lencz, T. (2021). Screening embryos for polygenic conditions and traits: Ethical considerations for an emerging technology. Genetics in Medicine, 23(3), 432-434.
- Lencz, T., Backenroth, D., Guna-Vazquez, E., Lambert, C., Buxbaum, J. D., Bhatt, S., ... and Lazaro-Munoz, G. (2022). Concerns about the use of polygenic embryo screening for psychiatric and cognitive traits. The Lancet Psychiatry, 9(10), 838-844.
- Lombardo, P. A. (2018). The power of heredity and the relevance of eugenic history. Genetics in Medicine, 20(11), 1305-1311.
- Martin, A. R., Kanai, M., Kamatani, Y., Okada, Y., Neale, B. M., and Daly, M. J. (2019). Clinical use of current polygenic risk scores may exacerbate health disparities. Nature Genetics, 51(4), 584-591.
- Miller, P. S., and Levine, R. L. (2013). Avoiding genetic genocide: Understanding good intentions and eugenics in the complex dialogue between the medical and disability communities. Genetics in Medicine, 15(2), 95-102.
- Polyakov, A., Amor, D. J., Savulescu, J., Gyngell, C., Georgiou, E. X., Ross, V., Mizrachi, Y., and Rozen, G. (2022). Polygenic risk score for embryo selection - not ready for prime time. Human Reproduction, 37(10), 2229-2236.
- Savulescu, J. (2007). In defence of procreative beneficence. Journal of Medical Ethics, 33(5), 284-288.
- Turley, P., Meyer, M. N., Wang, N., Cesarini, D., Hammonds, E., Martin, A. R., ... and Visscher, P. M. (2021). Problems with using polygenic scores to select embryos. New England Journal of Medicine, 385(1), 78-86.
Insights, Analysis, and Developments
Editorial Note: As polygenic embryo screening moves from research laboratories into fertility clinics, the gap between what the technology promises and what it can reliably deliver remains wide - and the ethical terrain it occupies grows more complex by the year. The disability community, psychiatric advocates, and geneticists alike are calling for regulatory frameworks that match the pace of innovation, insisting that decisions about which lives are worth bringing into the world should never be reduced to a statistical score alone. Author Credentials: Ian is the founder and Editor-in-Chief of Disabled World, a leading resource for news and information on disability issues. With a global perspective shaped by years of travel and lived experience, Ian is a committed proponent of the Social Model of Disability-a transformative framework developed by disabled activists in the 1970s that emphasizes dismantling societal barriers rather than focusing solely on individual impairments. His work reflects a deep commitment to disability rights, accessibility, and social inclusion. To learn more about Ian's background, expertise, and accomplishments, visit his full biography.
Author Credentials: Ian is the founder and Editor-in-Chief of Disabled World, a leading resource for news and information on disability issues. With a global perspective shaped by years of travel and lived experience, Ian is a committed proponent of the Social Model of Disability-a transformative framework developed by disabled activists in the 1970s that emphasizes dismantling societal barriers rather than focusing solely on individual impairments. His work reflects a deep commitment to disability rights, accessibility, and social inclusion. To learn more about Ian's background, expertise, and accomplishments, visit his full biography.